


Gum disease (also called periodontal disease) is an infection and inflammatory process that affects the gums and the bone that supports your teeth. It often begins subtly—like bleeding while brushing— but if it advances, it can lead to gum recession, loose teeth, and bone loss. At Diamond Dental Arts, we focus on early detection, personalized treatment, and long-term maintenance.
Call or text: (941) 637-0101

Gum disease is caused by bacterial buildup that triggers inflammation in the gums and can eventually affect the bone around the teeth. In the beginning, the infection may look like mild redness or bleeding. If it continues untreated, the gums can start separating from the teeth, forming deeper pockets that trap bacteria and become difficult to clean at home.
The earlier gum inflammation is addressed, the easier it is to stabilize the tissues and reduce long-term risks like recession and bone loss.

Gum disease generally develops in stages. The earliest stage is gingivitis, where the gums become irritated, swollen, and may bleed—especially during brushing or flossing. Gingivitis is often reversible with professional cleaning and better home care.
The more advanced stage is periodontitis. At this point, the infection can damage the supporting bone and fibers around the teeth. The gums may pull away, pockets deepen, and teeth can begin to feel loose over time.
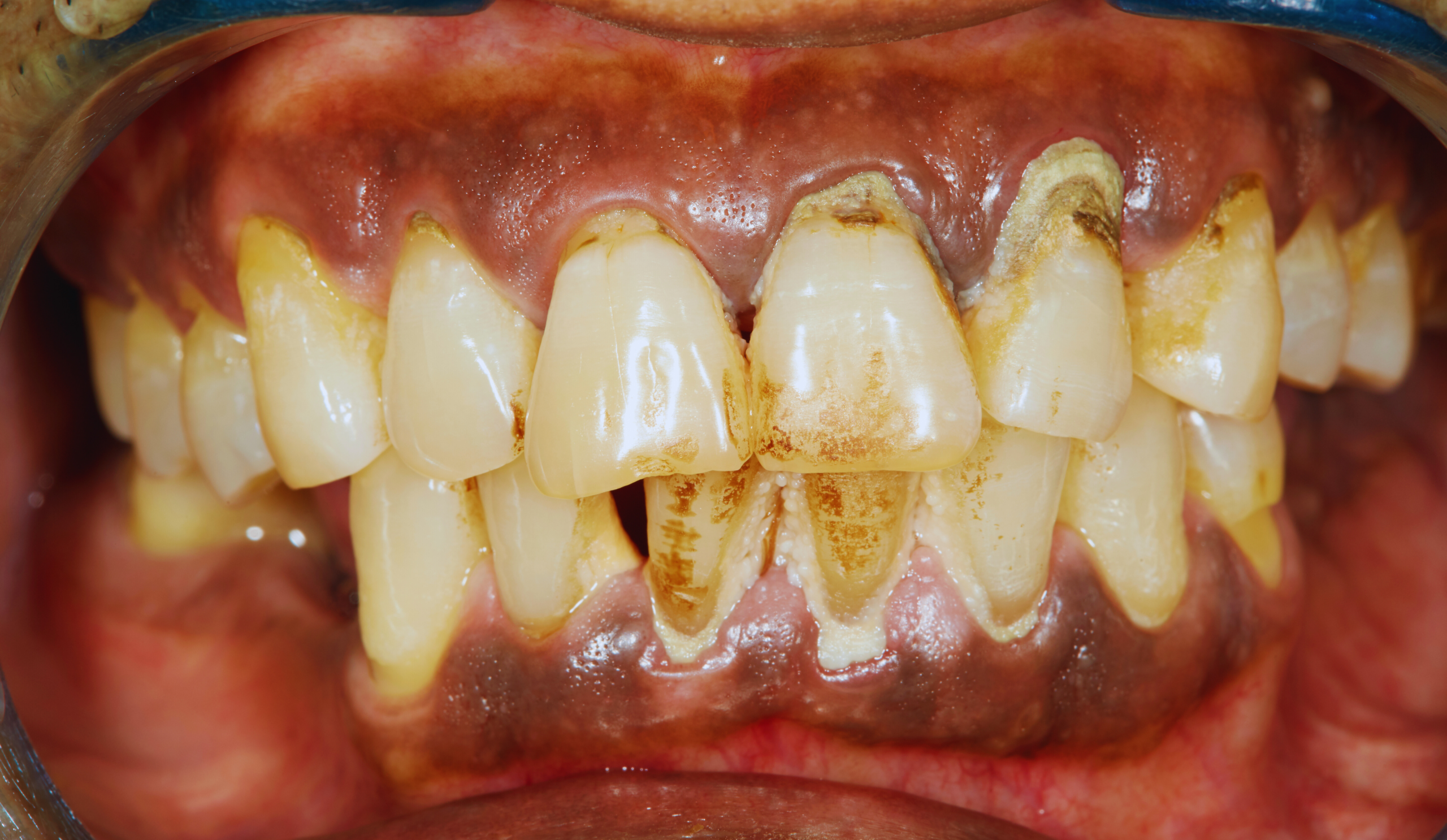
Gum disease begins when bacteria remain on the teeth long enough to form a sticky film called plaque. If plaque is not removed consistently, it can harden into tartar (also called calculus). Tartar can extend below the gumline, making the teeth much harder to clean on your own.
Once tartar is present, professional care is needed to remove it and reduce infection. That’s why regular cleanings and exams are a key part of prevention.
Gum disease often progresses quietly. If you notice any of the following, it’s a good idea to schedule an evaluation:
• Ongoing bad breath or a persistent bad taste
• Red, puffy, tender, or bleeding gums
• Discomfort when chewing
• Teeth that feel loose or more sensitive than usual
• Gums pulling away (receding) or teeth looking “longer”
• Changes in how your teeth fit together when you bite
• Partial dentures or bridges that suddenly feel different
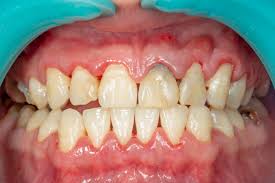
Several factors can make gum disease more likely or harder to control. Some of the most common include smoking, diabetes, inconsistent home care, family history, crowded or crooked teeth that are harder to clean, immune system concerns, and medications that reduce saliva (dry mouth). Hormonal changes can also make gums more reactive and easier to inflame.
Gum recession happens when the gumline gradually pulls back, exposing more of the tooth (or the root). This can create small gaps where bacteria collect more easily. Many people first notice recession as sensitivity, or they may feel a small notch near the gumline.
Recession isn’t only cosmetic—exposed roots are more vulnerable to decay and can lose support over time. If you think your gums are receding, it’s important to be evaluated so we can identify the cause and protect the area.
• Periodontal infection that damages gum and bone support
• Plaque/tartar buildup at the gumline
• Brushing too aggressively or with a hard brush
• Bite forces or clenching/grinding in some cases
Gum disease can often be controlled with a strong daily routine plus consistent professional care. For mild inflammation, regular cleanings and better brushing/flossing technique may be enough to restore healthier gums. More advanced cases may require deep cleaning below the gumline and a structured maintenance schedule to keep bacteria down.
In certain situations, additional supportive care may be recommended, such as localized antimicrobial therapy or other periodontal services based on your needs.
Brush twice daily (focus at the gumline), clean between teeth daily, and keep your checkups consistent— especially if you’ve had bleeding gums, recession, or a history of gum disease.
Questions or ready to schedule, call (941) 637-0101
